
Whether you are lost in the wilderness, stuck at home in a grid down situation, or you’re slogging through a cold weather bug out scenario, chilly conditions will give you some extra problems to face. Extra problems above and beyond your typical survival priorities.
While there are many cold weather threats in winter conditions, the following six hazards are the most likely threats you’ll face in the wintertime. Don’t become a casualty of the cold by learning to identify and treat these common winter injuries and ailments.
Hypothermia
Hypothermia is a medical condition in which the victim’s body gets too cold to function correctly. This can lead to death. This low temperature in the body’s core can be caused by exposure to water, wind, very cold air, or a combination of these elements. Eating ice or snow for hydration can also push someone over the edge toward a hypothermic state. Ice and snow should always be melted back into water before consumption.

Staying alert to the threat of a cold body core is an important way to keep out of trouble. Watch for the signs of hypothermia as it’s important to catch while still treatable in the field. The symptoms of hypothermia are diverse, but a person typically starts shivering as the body attempts to generate more heat, their faculties become impaired, the mind and motor skills fail, and they get sleepy.
They may also cast off their clothing as their frigid skin feels “hot” and their sluggish mind doesn’t understand the peril. Some hypothermia victims are located by the trail of discarded clothing that leads to their frozen body. Grim stories, but true, and you need to know the risk. If a person gets very cold, stops shivering and falls asleep, they’ll likely die without swift and correct medical intervention. Follow the symptoms through this chart to better understand how the body reacts to this cold weather crisis.
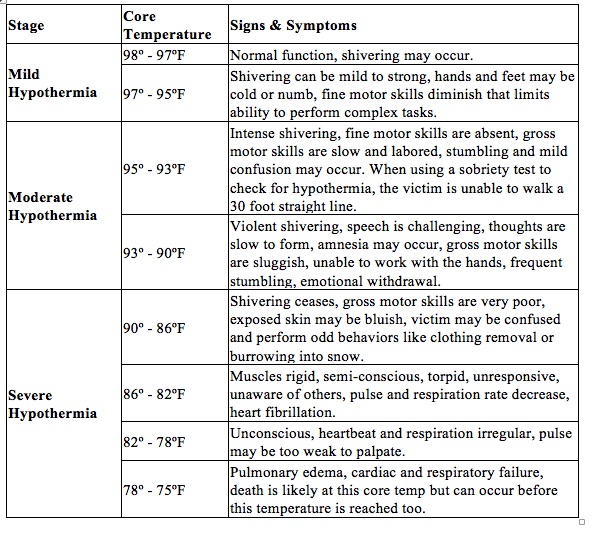
Test For Early Hypothermia
Keeping an eye out for shivering in yourself and your group is a great step toward hypothermia prevention. I like to supplement this vigilance with a quick assessment for fine motor skills, one that can be performed at any time in cold conditions. Simply touch the tip of your thumb to the tip of each of your fingers on the same hand, with or without gloves.
Assuming you can touch your thumb to fingertips in warm weather, you should still be able to do this in cold weather. This full range of motion means that your forearms haven’t tightened up and you’re not hypothermic yet. Failure to be able to touch your thumb to pinky and ring finger means that muscles are tightening up. Stronger hypothermia symptoms such as shivering and clumsiness will soon follow.
Cut Your Losses
The first step in treating hypothermia at any stage is to reduce heat loss. For mild to moderate cases, add another layer of clothing or replace wet clothing with a dry set. Get the victim into some kind of shelter or help them stand near a warm fire. Don’t leave them alone because they can fall into the fire if they lose their balance.
For severe hypothermia, remove wet clothing and place them in a cocoon of warm gear. Use multiple sleeping bags, blankets, sleeping pads, space blankets, and any other insulting or reflective materials to aid the victim’s own heat generating abilities. You have to reduce the victim’s heat loss through conduction, convection, and radiation before rewarming can effectively help.
Give Fluid and Fuel
Rewarming someone is the main method of treatment for hypothermia victims. Most hypothermia patients (the conscious ones) get a big boost from fluid and fuel. A little high calorie food and some sips of a warm beverage. Something like hot chocolate will provide both calories and a heat source. This nourishment capitalizes on the victim’s own heat generating ability. Sweets like candy can give them a quick boost of energy but it fades fast.
What a person really needs is a blend of quick burning carbs, protein, and some slow burning fat. If the hypothermia is mild to moderate, give them hot fatty foods. Skip the alcohol, coffee, tea, and don’t let them smoke. Alcohol is a vasodilator that will increase peripheral heat loss. Caffeine is a diuretic that can aggravate dehydration. Worst of all, the nicotine in tobacco is a vasoconstrictor that increases the risk of frostbite.
Try External Rewarming
There are many ways to apply this technique but they all involve the use of supplemental heat sources to revive the victim. Mild hypothermia victims can take advantage of “body to body” contact while wrapped in insulating materials. No need to be naked, light clothing such as long johns can be worn. Just make sure the patient is dry. Polypropylene long johns as a base layer will minimize sweating on the skin while allowing external heat to come through.
Stronger hypothermia cases will respond well to warming devices such as a hot water bottle or warm stone. Put them in both armpits, in the groin, and on each side of the neck. This is used in tandem with an insulating cocoon of warm bedding.
For long lasting support, pour boiling water into a one liter bottle made from Lexan plastic or metal. These bottle types can handle the high temperature. Screw the lid on tightly and slide the bottle down into a thick sock. This insulated bottle won’t be too hot on the skin and will stay warm for several hours. Make several of these then place around the patient’s armpits, groin, and neck.
Watch For “Afterdrop”
Just when you think your patient is improving, there may be a situation where the core body temperature actually drops during the rewarming regimen. This happens as a result of the cold blood returning from peripheral vessels in the arms and legs as the rewarmed vessels dilate back to their normal size. When this cold and stagnant blood returns to the core, it can drop the temperature and cause other problems. This blood has been starved of oxygen and has undergone chemical changes which can actually cause cardiac arrhythmia or cardiac arrest.
Prevent afterdrop by rewarming the core only. Allow arms and legs to rewarm naturally and very slowly. Don’t rewarm the periphery or place the victim in a hot bath, hot tub, sauna, or any other extreme heat. Speaking of “dropping”, one final and little known fact about hypothermia is this, don’t ever drop a hypothermia victim. If you have to carry someone, do it with all possible caution. A sudden jolt to the chest, like a fall, can cause a fatal heart arrhythmia in a hypothermia victim.
Frostbite
Frostbite is the freezing of a portion of your body, typically due to inadequate insulation in subfreezing temperatures. It can also occur when restrictive clothing cuts off the circulation of warm blood to an extremity. Frostbitten flesh usually first appears as a white waxy looking patch on your skin. Most often it’s on the fingers, ears, nose, toes, or cheeks.
The area of frostbite can quickly grow in both size and seriousness if not thawed quickly. Ultimately this will lead to extensive tissue damage, loss of limbs, or worse. In extremely cold temperatures, especially those compounded by wind chill, you must be vigilant in preventing frostbite from occurring. It is far better to prevent frostbite in its early stages than be burdened with the care and treatment of badly frostbitten areas of your body.

Prevent frostbite by dressing appropriately for the conditions, staying dry, checking yourself and your group for the signs of frostbite regularly, and taking shelter when needed. Use a 3-layer clothing system. By adding and subtracting layers of clothing you can dial in the optimum comfort zone. Always wear a hat since 70% of body heat escapes from your head. Keep yourself a little on the cool side so you don’t allow your body to overheat and sweat.
Exercise extremities like your toes and fingers so that warm blood flows through them. Frequently check your ears, toes, fingers, and face to detect signs of frostbite. Areas of your body that become numb, tingling, or hard should be rewarmed immediately by using your warm hand, armpit, or another person’s warmth. Should a limb become frozen, you may have no choice but to prevent its thawing until rescued. You may be able to walk on a frozen foot but thawing it could render you immobile and unable to self-rescue.
Thaw frostbite ONLY if there is no danger of refreezing. Pre-medicate with pain relievers like Advil or Motrin, before you start thawing, as the pain will be intense. The prescription equivalent of Advil is 800 mg every 8 hours. Consult your doctor before taking larger than normal doses of OTC medicines. Deep frostbite requires hot water at stable temperatures, around 105 degrees F. Rewarm the tissue until it is soft and the color has returned.
NEVER use any heating devices, stoves, or fires to treat frostbite. Victims cannot feel the frostbitten tissue and can be burned easily.
Immersion Foot
An odd cousin to frostbite is immersion foot a.k.a. trench foot. It’s another form of tissue damage caused by the environment. This ailment happens during prolonged exposure to moisture and cold temperatures, even above freezing. It frequently occurs on the feet because wet boots and socks are typically the cause. The flesh of your feet will appear wrinkled, pale, and bloodless in the beginning stages. Then cold and numb feelings will increase as the skin turns red or blue.
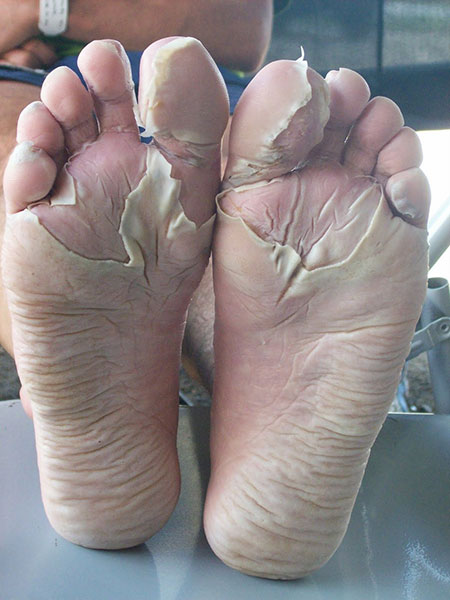
The affected limb will swell and stiffen to the point where walking is difficult. It’s important to take care of the feet since they are your life line to walking out of a survival situation. Immersion foot can become debilitating in just one day if it’s not properly taken care of and these conditions continue. Open sores may develop as the skin literally rots. This is why it’s often called “jungle rot” even in cold climates. Prevent immersion foot by keeping your feet warm and dry, change your socks frequently, massage your feet to rewarm and restore circulation regularly.
Snow Blindness
Something as simple as sunburn can become a real danger in cold winter conditions, especially if it’s in a vital area like your eyes. The strong winter sunlight bouncing off snow and ice causes intense UV light to strike exposed areas of your body that don’t usually get sun. Extra caution is needed in higher altitudes because the thinner air allows the passage of even more light. Open snowfields are another hazardous area on sunny days as they reflect light from all directions.
In addition to the possibility of sunburn on exposed skin, we also run the risk of receiving a sunburn in our eyes. Snow blindness is caused by the reflected glare of sunlight from snow, ice, water, and even light colored sand. The intense glare reflected from white snow on sunny days can make it very difficult to see. Keep in mind even the light from overcast skies can be reflected and magnified by the snow to put our eyes at risk. Snow blind eyes have actually become internally sunburned.
Symptoms of snow blindness include redness, puffiness around the eyes, intense burning, watering, and sensitivity to light. Victims describe a feeling of having sand or even broken glass in their eyes. There can be a temporary loss of vision or your eyes may even close up so that you are effectively blind. Becoming snow blind may also lead to painful headaches.

Snow blindness is easily avoided by wearing UV blocking sunglasses. Your winter survival kit should always include a pair as well as a small tube or stick of sun block for the other exposed areas of the body. Make a pair of snow goggles by cutting slits into a rectangular piece of bark, leather, or cloth then binding this over your eyes if necessary.
These slits will greatly reduce the amount of glare that strikes your eyes and help prevent snow blindness. In the event that you or someone in your group didn’t protect against snow blindness, the treatment is simply to rest in a dark place with covered eyes. You can also use analgesics to treat the pain. Vision will return in 12-18 hours even for the worst cases.
Dehydration
Dehydration can sneak up on you easily in winter. Cold air is often drier than the driest desert and it robs your body of moisture with every breath you take. This effectively makes winter survival as tough as desert conditions. But you may not feel thirsty even when your body requires more water than normal because of the cold air. To make matters worse, many tasks such as walking or working in snowy conditions will require much more effort.

This will further increase your water requirements. As you begin to slip into a dehydrated state, your energy level will drop and morale lower. The solution for this issue is simple, drink plenty of water at regular intervals. The test for proper hydration is simple too. Pay attention to your urine. You should be urinating every 2-3 hours, it should be light in color, and the volume should be more than a pint. If your urine is dark yellow, drink more water. If you haven’t peed all day, drink more water. Urine output is the best gauge of hydration. It factors in your activity level, health, and many other factors. If in doubt, drink even when you’re not thirsty.
Carbon Monoxide
Carbon monoxide poisoning is a dangerous hazard that can kill you in a very insidious way. Victims rarely ever realize that anything is wrong. It can happen in a cabin or home whenever there is a burning flame in an enclosed space without enough ventilation. You also run the risk of carbon monoxide poisoning by running a vehicle engine for warmth. Especially when the exhaust is partially blocked by mud, snow, water, or sand. The risk is particularly high during the cold winter months as we attempt to trap as much warmth as possible within our home or shelter.
Sources of carbon monoxide include woodstoves, gas heaters, and cooking fires. When a flame burns yellow, it’s emitting carbon monoxide. However, a blue flame is burning hot enough that it’s not emitting carbon monoxide. Always monitor the flame. Minor symptoms include a general feeling of tiredness, headache, and nausea. It’s important to note that you may not know anything is wrong until a collapse. Dying this way isn’t painful, but it’s still dying… Prevent this issue with adequate ventilation whenever you have any type of flame in an enclosed space. In a homebound survival setting, make sure you have fresh batteries in a smoke detector that also detects carbon monoxide.
Conclusion
It’s important to realize that snow and ice can be as dangerous as it is beautiful. It changes the dynamics of any survival situation. Snow can be effectively handled with some preparation and proper tool use.
